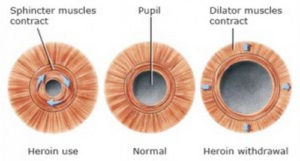 
With the continuing longer life expectancy, along with the increased diagnosis of BPH in older men, it is expected that patients on α1-ARA treatment requiring cataract surgery will continue to rise. Pharmacological inhibition of α1-ARA reduces the muscular tone and thus the pressure within prostatic urethra, and it is nowadays the first line medical approach to BPH. A study also reported drug-melanin interaction, which causes iris dilator muscle atrophy and therefore to IFIS. Furthermore, it was proposed that the long-term intake of α1-ARA may cause anatomical variations that are permanent and cannot be completely reversed with interruption of medication and is maintained despite the use of preoperative pharmacological dilation with topical cyclopentolate, phenylephrine and ketorolac. There is evidence that blocking α1 adrenergic receptors results in relaxation of the iris dilator muscle, with poor pupillary tone. α1-D contributes for spinal cord innervation and bladder muscle contraction. α1-B controls blood pressure through arterial smooth muscle relaxation and is highly present in the choroid (a highly vascularized tissue). The subtype α1-A is the main regulator of smooth muscle tone of the urinary system and of iris dilator muscle. There are 3 subtypes of α1-adrenergic receptors: α1-A, α1-B and α1-D. This inhibition can happen with the use of some types of medications, such as the most commonly prescribed α1-adrenegic receptor antagonist (α1-ARA) tamsulosin used for the management of benign prostatic hyperplasia (BPH). The most likely pathogenic mechanism for IFIS is the antagonism of α1-adrenergic receptors within the dilator muscle of the iris, which prevent the iris from dilation during surgery. The prevalence also varies among countries and is significantly increased in groups of patients with clinical factors positively correlated with IFIS.Ĭurrently in more recent studies, there is a tendency for higher rates of IFIS, perhaps due to the increasingly high prescription rate of medications associated with IFIS and also because of higher awareness and recognition of milder IFIS signs by surgeons. This wide range of prevalence might be due to the subjective clinical definition of this syndrome and its manifestations being a continuum of severity with variability between patients and between eyes of the same patient. The reported overall prevalence of IFIS in patients undergoing phacoemulsification is variable, ranging from 2% in the Chang and Campbell report in 2005, up to 12.6% in later studies. Therefore, it is important to anticipate IFIS and use pupil expansion devices as a preventive measure in the beginning of surgery rather than after IFIS has developed and the capsulorrhexis is already completed (which might compromise its integrity). 
diabetes), IFIS is characterized by an elastic iris which does not dilate with mechanical stretching. In contrast to other causes of small dilated pupil and progressive intraoperative miosis (e.g. Two additional pupil features may be present in IFIS: Propensity for iris prolapse toward the phaco and/or the side-port incisions Ī grading system for IFIS was suggested based on the presence of the previously described intraoperative signs as follows: no IFIS (stable iris without significant miosis), mild IFIS (noticeable floppy iris only), moderate IFIS (floppy iris and miosis) and severe IFIS (floppy iris, significant miosis and strong tendency to iris prolapse).Billowing of a flaccid iris stroma in response to ordinary intraocular fluid currents.This syndrome is known to cause a poor pupillary dilation, intraoperative complications during cataract surgery and is characterized by the following triad of intraoperative signs: Intraoperative floppy iris syndrome (IFIS) is a clinical entity originally described by Chang and Campbell in 2005. 1.5 Preoperative evaluation and preventive measures.1.4.7 Surgery (phacoemulsification) duration.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
